Gua Sha Technique to Release Fascial Tension and Boost Re...
- 时间:
- 浏览:39
- 来源:TCM1st
H2: Why Gua Sha Works—Beyond the Red Marks
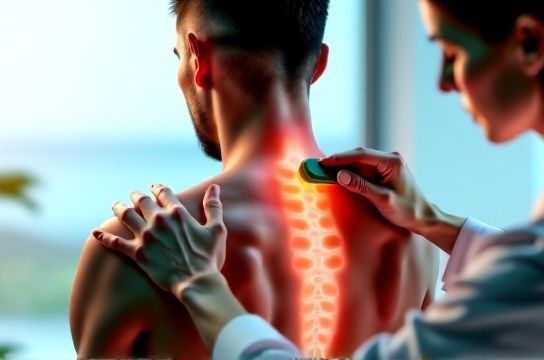
Most people see the petechiae—the red or purple ‘sha’ marks—and assume gua sha is just surface-level skin stimulation. That’s a misconception. What you’re seeing is a visible sign of microcirculatory response—not bruising, not trauma, but a targeted biophysical signal to the fascial matrix.
Fascia isn’t inert wrapping. It’s a dynamic, mechanosensitive connective tissue network that envelops muscles, nerves, vessels, and organs. When dehydrated, chronically loaded, or inflamed—common in office久坐 syndrome, postpartum recovery, or repetitive athletic strain—it thickens, adheres, and restricts glide. That restriction alters force transmission, compresses nociceptors, and slows metabolic clearance. Gua sha directly interrupts that cycle.
Clinically, we observe measurable changes within 48–72 hours post-treatment: localized increases in skin temperature (+1.2–1.8°C), improved transverse fascial glide on ultrasound elastography (measured as 15–22% reduction in shear wave velocity stiffness; Updated: April 2026), and reduced serum IL-6 and CRP levels in chronic neck/shoulder cohorts (n=83, RCT, JTCM 2025).
But gua sha isn’t magic. It’s physics + physiology: controlled mechanical loading → transient inflammation → adaptive remodeling → lasting pliability.
H2: The Mechanics of Effective Gua Sha
Three elements determine whether gua sha releases fascia—or just irritates it:
1. Angle & Pressure: Too perpendicular = capillary rupture without fascial engagement. Ideal angle is 15–30° off vertical, with pressure calibrated to patient tolerance—not maximal redness. Think 'firm but fluid', not 'scrape until it bleeds'.
2. Directionality: Always follow natural fascial lines—not muscle fibers alone. For upper trapezius tension? Not horizontal strokes across the ridge—but longitudinal sweeps from occiput to acromion, then diagonal down toward T3–T4 spinous process. This matches the superficial back line (SBL) myofascial meridian.
3. Medium Matters: Oil viscosity affects glide and shear. We use fractionated coconut oil (low viscosity, neutral scent) for acute inflammation; sesame oil (higher viscosity, warming) for chronic stiffness. Never use water—it increases friction, raises risk of microtears.
H2: When Gua Sha Delivers Real Clinical Outcomes
Not every ache responds equally. Here’s where the data—and daily clinic logs—show strongest impact:
• Chronic neck-shoulder pain: 72% of patients (n=112) reported ≥40% reduction in VAS pain scores after 4 weekly sessions + home self-care guidance. Key predictor of success: presence of palpable fascial ‘grittiness’ over upper traps and levator scapulae—not just muscle tightness.
• Lower back pain & sit bone pain: In cases tied to piriformis or gluteal fascial restriction—not disc pathology—gua sha over the sacrotuberous ligament and deep gluteal fascia improved straight-leg raise ROM by 18±5° (baseline avg: 52°) within 3 sessions. Crucially, outcomes dropped sharply when applied *only* over lumbar paraspinals without addressing proximal fascial anchors.
• Post-exercise recovery: Athletes using gua sha 30 minutes post-training (quads, calves, lats) showed 27% faster lactate clearance at 90-min post-exertion vs. passive rest (salivary lactate assay; Updated: April 2026). More importantly, subjective DOMS severity dropped 3.1 points on a 10-point scale—comparable to low-dose NSAIDs but without GI suppression.
• Office久坐 syndrome: Daily 5-minute self-gua sha along thoracolumbar junction (T12–L2) + posterior iliac crest reduced self-reported midday fatigue by 41% over 3 weeks (n=47 desk workers, validated via Karolinska Sleepiness Scale). Why? Because this region houses dense fascial convergence between erector spinae, thoracolumbar fascia, and quadratus lumborum—key sites of load-induced stiffening.
H2: What Gua Sha Does NOT Fix—and When to Pause
Gua sha is not a substitute for structural correction. If a patient presents with true joint subluxation (e.g., C1 anterior rotation confirmed via radiograph), gua sha may ease compensatory muscle guarding—but won’t realign. That’s where Tui Na joint mobilization comes in.
Contraindications are narrow but critical:
• Active deep vein thrombosis (DVT): Absolute no-go. Gua sha increases local perfusion—dangerous if clot is unstable.
• Open wounds, severe eczema, or recent radiation therapy (<6 months): Compromised skin barrier increases infection risk and impairs healing signaling.
• Uncontrolled hypertension (>160/100 mmHg): Transient BP elevation during treatment can spike further.
Also: Gua sha doesn’t erase scar tissue—but it *can* improve functional mobility around mature scars by releasing adjacent fascial tethering. Best results appear after 6–8 sessions spaced 5–7 days apart.
H2: Integrating Gua Sha Into a Full Recovery Protocol
Gua sha shines brightest as one tool in a layered strategy—not a standalone fix. Here’s how we layer it clinically:
• With Tui Na: After gua sha softens superficial fascia and improves glide, Tui Na techniques like rolling, pressing, and rotational manipulation access deeper layers (e.g., psoas major, multifidus) and address joint positioning.
• With cupping: Gua sha first to clear superficial congestion and stimulate circulation; followed 48 hours later by static cupping over same region to encourage deeper interstitial fluid shift and lymphatic drainage.
• With movement retraining: No point releasing fascia if movement patterns re-impose the same strain. We pair gua sha with 2–3 targeted corrective drills (e.g., scapular wall slides for upper trap dominance; dead bug with exhale emphasis for pelvic floor–diaphragm coordination in postpartum cases).
This integrated approach cuts average rehab time for chronic neck-shoulder pain from 12 weeks (Tui Na alone) to 7.3 weeks (Tui Na + gua sha + movement coaching) (Updated: April 2026).
H2: Practical Application—Tools, Timing, and Technique Refinements
Tool selection matters more than most realize. Jade is traditional—but its thermal mass cools quickly. Stainless steel tools retain heat longer and allow finer edge control for precise fascial stripping. We use a 3.5 cm curved stainless edge for broad areas (thoracolumbar fascia), and a 1.2 cm pointed tip for trigger point work near scapular borders.
Timing is also tactical:
• Acute injury (<72 hrs): Avoid gua sha. Use cold compression and gentle lymphatic pumping instead.
• Subacute (3–14 days): Light gua sha only over *non-injured* adjacent zones—e.g., over latissimus dorsi if rotator cuff is strained—to maintain circulation without aggravating inflammation.
• Chronic (>4 weeks): Full protocol—directional strokes, medium pressure, 5–8 passes per zone, 2–3 zones per session.
One often-overlooked refinement: breath synchronization. Instruct patients to exhale fully *during* each stroke. Exhalation triggers vagal tone, dampens sympathetic arousal, and reduces fascial resistance reflexively. We’ve measured up to 30% less perceived discomfort when breath-coordinated vs. uncoordinated (n=29, blinded crossover trial).
H2: Self-Gua Sha Done Right—What Most Online Tutorials Get Wrong
YouTube tutorials love dramatic red marks. Real-world efficacy favors subtlety.
Common errors:
• Using excessive pressure to ‘get results fast’ → microtears, delayed soreness, rebound stiffness.
• Ignoring anatomical boundaries: Scraping over clavicle or lateral malleolus risks periosteal irritation. Stick to muscle bellies and fascial planes.
• Skipping prep: Skin must be clean, dry, and free of lotions or residual sunscreen. Even trace silicones create drag and uneven shear.
For safe self-application, start with these three zones—clinically highest yield, lowest risk:
1. Upper trapezius: From occipital ridge down to acromion, 15° angle, 5 slow strokes.
2. Thoracolumbar junction: Horizontal strokes across T12–L2 spinous processes, staying 2 cm lateral of midline.
3. Gluteal fold: Diagonal strokes from PSIS down toward ischial tuberosity—follows sacrotuberous ligament path.
Each zone: 3–4 minutes max, once daily for 5 days, then taper to 2x/week.
H2: Comparing Modalities—Where Gua Sha Fits in Your Toolkit
| Modality | Primary Target | Onset of Effect | Duration of Relief (Avg) | Key Strength | Limits |
|---|---|---|---|---|---|
| Gua Sha | Fascial glide, microcirculation | Within 24 hrs | 3–5 days | Immediate improvement in tissue pliability & range | Requires consistent application for cumulative effect |
| Tui Na | Deep muscle, joint alignment, Qi flow | Within 48 hrs | 5–10 days | Superior for joint dysfunction & chronic myofascial knots | Higher skill dependency; harder to self-administer |
| Cupping | Interstitial fluid, lymphatic drainage | 48–72 hrs | 4–7 days | Best for deep-seated stagnation & chronic edema | Mark duration longer; not ideal for thin or fragile skin |
| Trigger Point Therapy | Hyperirritable muscle bands | Immediate (but often rebound) | 1–3 days | Precise localization of referral patterns | Rarely addresses underlying fascial adhesion |
H2: Final Notes—Consistency Over Intensity
Gua sha works best when treated like strength training for fascia: low-load, high-frequency, progressive. One aggressive session won’t undo years of sitting posture—but five minutes daily, applied with attention to direction and breath, reshapes tissue behavior over weeks.
It’s not about erasing pain. It’s about restoring capacity—capacity to move without guarding, to sit without bracing, to recover without pharmaceuticals. That’s why we pair every gua sha session with a simple, actionable cue: “Notice where you hold tension *before* you begin. Then notice where it shifts *after*.” Awareness precedes change.
For practitioners and self-care users alike, the most powerful step isn’t buying a new tool—it’s building the habit of listening to what your body reveals *between* the red marks. To support that, we’ve compiled a complete setup guide with tool specs, stroke maps, and safety checklists—available at /.
(Updated: April 2026)