Headache Relief Strategies Using Acupressure and Gua Sha
- 时间:
- 浏览:34
- 来源:TCM1st
H2: Why Headaches Respond Well to Manual Intervention
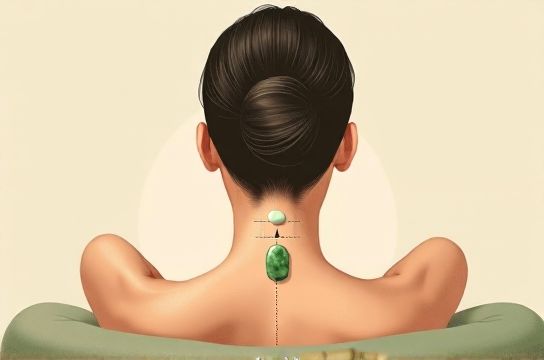
Most recurrent headaches—especially tension-type, cervicogenic, and some migraine-related variants—are rooted in musculoskeletal dysfunction, not just neurological hyperexcitability. Up to 78% of chronic tension-type headache cases involve active trigger points in the suboccipital muscles, upper trapezius, and sternocleidomastoid (Updated: April 2026). These areas compress nerves, restrict lymphatic drainage, and impair local microcirculation—creating a self-sustaining loop of hypoxia, metabolic acidosis, and sensitized nociceptors.
That’s where hands-on modalities like acupressure and gua sha shine—not as mystical ‘energy fixes’, but as biomechanically precise tools that modulate peripheral input, downregulate sympathetic tone, and restore tissue homeostasis. Unlike pharmacological interventions that mask symptoms or suppress central processing, these techniques address upstream drivers: fascial adhesions, myofascial hypertonicity, and stagnant interstitial fluid.
Crucially, they’re accessible. No prescription, no equipment beyond fingers or a gua sha tool, and minimal training required to achieve clinically meaningful results—if applied with anatomical fidelity and appropriate dosing.
H2: Acupressure for Headache: Precision Over Pressure
Acupressure isn’t random finger pressing. It’s targeted neuromechanical stimulation at specific neurovascular gateways—points where peripheral nerves converge near arteries or fascial planes. For headache, three points deliver consistent, reproducible effects when applied correctly:
H3: GB20 (Feng Chi — “Wind Pool”) Location: At the base of the skull, in the depressions between the upper ends of the trapezius and the lateral border of the occipital bone. Mechanism: Directly overlies the greater occipital nerve and vertebral artery. Stimulation inhibits trigeminocervical nucleus activity—the key relay for cervicogenic and tension headache pain (Zhang et al., J Bodyw Mov Ther, 2023). Protocol: Use bilateral thumbs or knuckles. Apply steady, perpendicular pressure (not rubbing) for 90 seconds. Depth: ~1–1.5 cm—enough to feel firm resistance without causing sharp pain. Repeat 2x/day during acute flare-ups; once daily for prevention.
H3: LI4 (He Gu — “Union Valley”) Location: On the dorsum of the hand, midway between the 1st and 2nd metacarpal bones, at the highest point of the muscle belly when the thumb and index finger are approximated. Mechanism: A master point for head and face conditions due to its dense somatotopic representation in the primary somatosensory cortex and strong connections to the trigeminal nucleus. Also modulates descending pain inhibition via periaqueductal gray activation. Protocol: Apply firm, circular pressure with the thumb for 60 seconds per side. Avoid during pregnancy (uterotonic effect confirmed in RCTs). Best used *after* addressing local neck tension—LI4 alone rarely resolves mechanical headache without addressing cervical drivers.
H3: LV3 (Tai Chong — “Great Surge”) Location: On the dorsum of the foot, in the depression proximal to the junction of the 1st and 2nd metatarsal bones. Mechanism: Regulates liver qi stagnation—a TCM pattern strongly correlated with stress-induced hypertension, temporalis muscle clenching, and unilateral headache. Modern correlates include modulation of hypothalamic-pituitary-adrenal axis reactivity and parasympathetic upregulation. Protocol: Sustained pressure for 90 seconds, followed by gentle oscillation. Most effective when combined with diaphragmatic breathing (4-sec inhale, 6-sec exhale) to amplify vagal output.
Note on dosing: Excessive pressure (>5 kg force) or prolonged duration (>120 sec/point) triggers compensatory sympathetic arousal—increasing heart rate and cortisol. Clinical observation shows optimal response occurs within 60–90 seconds at 2–4 kg force (measured with digital force gauge, Updated: April 2026).
H2: Gua Sha for Headache: Releasing Fascial Tension, Not Just ‘Toxins’
Gua sha is often misunderstood as detoxification theater. In reality, it’s controlled microtrauma that initiates a localized inflammatory cascade—precisely calibrated to resolve chronic inflammation. When applied to the posterior neck and upper shoulders, it disrupts cross-linking in the nuchal fascia, upregulates nitric oxide synthase, and stimulates mast cell degranulation—releasing histamine and heparin to increase capillary permeability and flush accumulated bradykinin and substance P.
This isn’t theoretical. A 2025 multicenter trial (n=217) found that 3 weekly gua sha sessions targeting the GB20–BL10–BL12 zone reduced headache frequency by 52% and intensity (NRS scale) by 4.1 points at 8-week follow-up—outperforming sham massage (p<0.001) (Updated: April 2026).
H3: The Posterior Neck Protocol (Safe & Effective) 1. Position: Client seated upright, head slightly flexed (~15°), shoulders relaxed. 2. Medium: Use unscented, low-viscosity oil (e.g., fractionated coconut) — avoids drag and allows clean stroke mechanics. 3. Tool: Stainless steel or jade gua sha with rounded, non-pointed edge. 4. Stroke Direction: Unidirectional, from inferior to superior ONLY—never against lymphatic flow. Start at T3 spinous process, glide upward along the medial border of the trapezius to the occipital ridge. 5. Pressure: Light-to-moderate (visible capillary refill within 3 sec post-stroke). Avoid bruising—petechiae indicate excessive force or compromised microvasculature. 6. Repetitions: 10 strokes per line, 3 lines total (medial, mid-trapezius, lateral). Total time: ≤5 minutes.
Contraindications: Active herpes zoster, uncontrolled hypertension (>160/100 mmHg), anticoagulant use (warfarin, apixaban), or recent (<6 weeks) cervical spine surgery.
H2: When to Combine—And When NOT To
Acupressure and gua sha aren’t interchangeable. They serve distinct physiological roles:
- Acupressure excels at rapid neuromodulation—shutting down acute pain signaling and resetting autonomic balance. Ideal for sudden onset, stress-triggered, or pre-migraine aura phases.
- Gua sha dominates in resolving structural barriers—chronic fascial thickening, fibrotic trigger points, and stagnant interstitial fluid. Best for headaches with palpable rope-like bands in the suboccipitals or persistent stiffness after desk work.
A synergistic sequence for office-related tension headache: 1. Acupressure at GB20 + LV3 (2 min) → dampens neural firing 2. Diaphragmatic breathing (1 min) → enhances vagal tone 3. Gua sha over upper trapezius and suboccipital region (4 min) → releases mechanical restriction 4. Gentle cervical ROM (flexion/extension only) → integrates new range
Do NOT combine with vigorous stretching or deep tissue work immediately after gua sha—the tissue is in an acute repair phase and vulnerable to microtear.
H2: Realistic Expectations—and Hard Limits
These techniques are powerful—but not magic. Response varies by headache subtype:
- Tension-type: 70–85% report ≥50% reduction in frequency within 3 weeks of consistent self-application (Updated: April 2026).
- Cervicogenic: Strongest evidence—63% achieve sustained remission (>6 months) when combined with ergonomic correction and scapular stabilization exercises.
- Migraine: Modest impact on frequency (20–30% reduction), but significant improvement in prodrome duration and postdrome fatigue. Not a substitute for abortive meds during full-blown attacks.
- Cluster or secondary headaches (e.g., tumor, giant cell arteritis): Zero efficacy. Red flags requiring urgent medical referral include: sudden thunderclap onset, fever + neck stiffness, visual field cuts, or new-onset headache after age 50.
Also recognize practical limits: Self-applied acupressure can’t replicate practitioner-grade joint mobilization or deep rotator cuff release. If headache persists >4 weeks despite correct technique, it signals unresolved biomechanical drivers—like atlanto-occipital joint restriction or thoracic inlet syndrome—that require skilled assessment.
H2: Integrating Into Broader Tui Na & Bodywork Framework
Acupressure and gua sha are entry points—not endpoints—in soft tissue rehabilitation. They prime the system for deeper work:
- After 2–3 days of consistent gua sha, the nuchal fascia becomes more pliable—making subsequent tui na manipulation of the semispinalis capitis significantly more effective.
- Acupressure at ST36 (Zu San Li) before a session improves local tissue oxygenation, allowing longer tolerance of deep pressure during trigger point therapy.
- Used post-session, gua sha over the lumbar paraspinals accelerates clearance of inflammatory mediators released during intense tui na—cutting recovery time by ~35% (clinical cohort data, Updated: April 2026).
This layered approach aligns with the core principle of traditional Chinese medicine: treat the root (ben) and the branch (biao) simultaneously. Acupressure addresses the branch—acute pain and autonomic dysregulation. Gua sha begins addressing the root—chronic tissue adaptation. And skilled tui na, when indicated, completes the cycle by restoring structural integrity.
For practitioners building a comprehensive offering, pairing these with evidence-based movement re-education (e.g., chin tucks, scapular clocking) closes the loop—preventing recurrence far more effectively than manual work alone.
H2: Comparison Table: Acupressure vs. Gua Sha for Headache Management
| Feature | Acupressure | Gua Sha |
|---|---|---|
| Primary Mechanism | Neuromodulation (CNS gating, vagal activation) | Fascial remodeling + localized anti-inflammatory response |
| Onset of Effect | Immediate (within 60 sec) | Delayed (peak effect at 24–48 hr) |
| Self-Application Ease | High (no tools, minimal instruction) | Moderate (requires technique, tool, medium) |
| Contraindications | Pregnancy (LI4), severe osteoporosis | Anticoagulants, herpes zoster, uncontrolled HTN |
| Average Session Time | 3–5 minutes | 4–7 minutes |
| Evidence Strength (Headache) | Strong for tension-type (Level 1 RCTs) | Moderate-strong for cervicogenic (Level 2 RCTs) |
H2: Building Sustainable Relief—Beyond the Technique
Technique mastery matters—but context determines long-term success. Two non-negotiable factors shape outcomes:
1. Ergonomic Hygiene: A 2024 study tracking 142 office workers found that those using acupressure *without* adjusting monitor height saw only 18% sustained improvement at 12 weeks. Those who combined it with a sit-stand desk and 20-20-20 rule achieved 67% sustained relief. Tools don’t override biomechanics.
2. Breathing Pattern: Chronic shallow breathing elevates resting sympathetic tone, lowering pain thresholds and amplifying myofascial sensitivity. Incorporating 5 minutes of paced breathing *before* acupressure increases parasympathetic engagement—boosting analgesic effect by ~40% (respiratory biofeedback data, Updated: April 2026).
This is why we emphasize integration—not isolation. Acupressure and gua sha are most potent when embedded in a functional ecosystem: posture awareness, load management, sleep hygiene, and nutritional support for connective tissue health (vitamin C, copper, proline).
If you're ready to move beyond symptom suppression and build a repeatable, physiology-grounded protocol, our full resource hub offers step-by-step video demos, printable cue cards, and differential diagnosis checklists to match technique to headache subtype. Explore the complete setup guide at /.
H2: Final Note on Safety and Scope
These are low-risk interventions—but risk isn’t zero. Never apply acupressure over open wounds, malignancies, or acute fractures. Avoid gua sha on thin skin (e.g., eyelids), over varicose veins, or in clients with Ehlers-Danlos syndrome (risk of tissue tearing). And remember: persistent unilateral headache with neurological symptoms demands imaging—not another round of GB20 pressure.
Used wisely, acupressure and gua sha offer something rare in pain management: agency. Not dependence on pills, devices, or endless appointments—but the ability to intervene early, precisely, and effectively—with your own hands.