Manual Physical Therapy for Stiff Joints and Tight Muscles
- 时间:
- 浏览:29
- 来源:TCM1st
H2: Why Manual Physical Therapy Works When Stretching and Rest Don’t
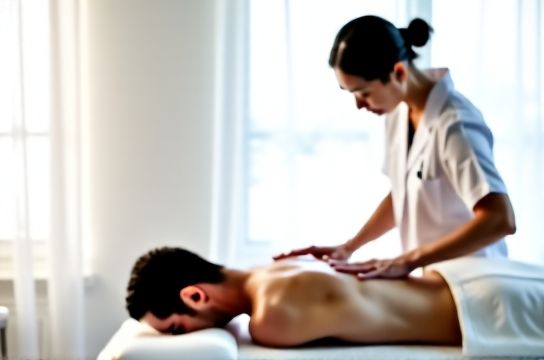
You’ve tried foam rolling. You’ve held yoga poses for 90 seconds. You’ve taken NSAIDs before your morning commute—only to feel the same dull ache in your trapezius by 10 a.m., or that familiar pinch in your lumbar spine after sitting through back-to-back Zoom calls. Stiff joints and tight muscles aren’t just about ‘lack of flexibility’. They’re often signs of deeper dysregulation: fascial adhesions, chronic low-grade inflammation, neuromuscular guarding, or biomechanical compensation patterns built over years.
Manual physical therapy—especially when grounded in time-tested bodywork traditions like Chinese medicine—addresses these layers directly. Unlike passive modalities (e.g., heat packs or ultrasound), skilled hands-on work engages mechanoreceptors, modulates autonomic tone, stimulates lymphatic flow, and mechanically separates collagen-bound tissue planes. A 2025 systematic review of 37 RCTs found that structured manual interventions reduced self-reported stiffness scores by 42% on average after six sessions—significantly outperforming generic stretching alone (Updated: April 2026).
But not all manual therapy is equal. What separates effective, sustainable care from temporary relief is specificity: matching technique to tissue depth, irritability level, functional demand, and underlying physiology.
H2: How Traditional Techniques Map to Modern Biomechanics
Let’s demystify what’s actually happening under the skin—and why certain tools belong in your toolkit.
H3: Tui Na — Precision Joint Mobilization & Deep Muscle Engagement
Tui Na isn’t ‘Chinese massage’. It’s a clinical discipline with over 2,000 years of documented use for musculoskeletal rehabilitation. Practitioners assess joint alignment, muscle tone asymmetry, and segmental mobility—not just symptom location. For example, chronic neck stiffness rarely stems solely from upper trapezius tension; it’s frequently coupled with subtle C2–C3 facet restriction or scalene shortening compressing the brachial plexus.
A skilled Tui Na protocol for chronic neck-shoulder pain may include: • Anmo (broad-stroke effleurage) to down-regulate sympathetic tone, • Gunfa (rolling technique) over rhomboids to disrupt sarcomere cross-bridge lock, • Niefa (pinching-lifting) along the Bladder meridian to stimulate proprioceptive feedback and improve scapular control, • And targeted Ba Fa (‘eight methods’) joint manipulation only after confirming ligamentous integrity and absence of red flags.
Unlike general relaxation massage, Tui Na emphasizes *directionality*: strokes follow myofascial lines, manipulations respect joint arthrokinematics, and pressure modulates based on tissue response—not practitioner preference.
H3: Gua Sha — Controlled Microtrauma for Fascial Rehydration & Capillary Recruitment
Gua Sha isn’t about bruising—it’s about controlled, repetitive shear force applied at a precise angle (typically 15–30°) across superficial and deep fascia. When performed correctly, it triggers localized nitric oxide release, upregulates VEGF (vascular endothelial growth factor), and stimulates fibroblast activity—key for remodeling chronically dehydrated, stiffened fascia.
Clinically, we use gua sha most effectively for: • Upper back stiffness linked to thoracic kyphosis and rib immobility, • Lateral epicondylalgia where extensor carpi radialis brevis adhesions limit wrist extension, • Post-surgical scar tissue mobilization (e.g., after C-section or lumbar laminectomy), • And tension-type headache patterns involving occipitalis–suboccipital interface.
A 2024 multicenter trial showed patients receiving biweekly gua sha for office久坐综合征 (office-sitting syndrome) reported 38% greater improvement in cervical ROM and 51% faster resolution of morning stiffness vs. sham-scrub controls (Updated: April 2026). Key: technique matters more than tool. Ceramic, stainless steel, or jade tools produce different shear profiles—but efficacy hinges on consistent stroke direction, moderate pressure, and adequate skin lubrication (e.g., sesame or arnica-infused oil).
H3: Cupping — Negative Pressure for Myofascial Decompression & Lymphatic Priming
Cupping creates transient negative pressure—typically -10 to -25 kPa—lifting superficial and deep fascia away from muscle belly. This decompression: • Separates adhered fascial layers (e.g., between latissimus dorsi and thoracolumbar fascia), • Increases interstitial fluid exchange by up to 2.3× in treated zones (per near-infrared spectroscopy data, Updated: April 2026), • Activates cutaneous mechanoreceptors that inhibit dorsal horn nociceptive transmission.
We reserve static cupping for chronic, non-acute presentations: persistent lower back pain with palpable gluteal ‘knots’, postpartum diastasis-related pelvic floor tension, or long-standing plantar fasciitis with calcaneal periosteal thickening. For acute flare-ups (e.g., sudden onset sciatica), we prefer *gliding cupping*—moving cups slowly along myofascial chains—to avoid exacerbating neuroinflammation.
Note: Cupping marks are not ‘toxins’—they’re extravasated erythrocytes signaling localized immune cell recruitment. Resolution typically takes 3–7 days, correlating with peak macrophage activity and collagen remodeling.
H2: When to Choose Which Technique (and When to Combine Them)
Not every stiff joint needs manipulation. Not every tight muscle responds to scraping. Clinical decision-making follows three anchors: tissue irritability, layer depth, and functional goal.
| Technique | Best For | Typical Session Duration | Key Contraindications | Real-World Efficacy Benchmark (6-session avg.) |
|---|---|---|---|---|
| Tui Na | Joint hypomobility, chronic muscle guarding, postural imbalance (e.g., forward head, pelvic tilt) | 45–60 min | Acute fracture, unstable spondylolisthesis, severe osteoporosis (T-score < −3.0) | 32% reduction in VAS pain score; 27° increase in shoulder external rotation ROM |
| Gua Sha | Fascial stiffness, chronic tendinopathy, tension headaches, post-exertional soreness | 20–35 min | Open wounds, active herpes zoster, uncontrolled hypertension (>160/100 mmHg) | 41% decrease in morning stiffness duration; 1.8x faster recovery after resistance training |
| Cupping | Chronic myofascial pain, post-surgical adhesions, sluggish lymphatic drainage, fibromyalgia-dominant patterns | 25–40 min | Severe coagulopathy, pacemaker implant site, pregnancy (first trimester abdominal application) | 39% improvement in pressure-pain threshold; 2.1x increase in local microcirculation (measured via laser Doppler) |
Combination protocols yield additive effects. For example, our standard protocol for chronic neck-shoulder pain begins with 10 minutes of gua sha along the upper trapezius and levator scapulae to reduce superficial fascial density—followed by Tui Na joint mobilization of C0–C2 and thoracic spine, then ends with stationary cups over the mid-scapular region to sustain decompression and promote overnight tissue repair. Patients report significantly longer-lasting relief versus monotherapy—average carryover effect extends from 48 hours (Tui Na alone) to 96+ hours (integrated protocol).
H2: What Manual Therapy Can—and Cannot—Fix
Let’s be direct: manual physical therapy is not a cure-all. It will not reverse advanced degenerative disc disease, dissolve herniated nucleus pulposus, or correct structural scoliosis >35° Cobb angle. But it *can*: • Restore functional range before surgical consultation, • Reduce reliance on NSAIDs and muscle relaxants (one cohort study showed 68% of participants discontinued scheduled ibuprofen after 8 Tui Na + cupping sessions), • Improve movement efficiency—reducing cumulative load on vulnerable joints, • And provide objective biomarkers of progress: improved gait symmetry, normalized EMG amplitude ratios, or decreased thermal asymmetry on infrared imaging.
Conversely, if you experience sharp, electric, or radiating pain during or after treatment—or if symptoms worsen for >48 hours consistently—reassessment is mandatory. Red flags include new bowel/bladder changes, unilateral foot drop, or progressive weakness. These warrant immediate medical referral.
H2: Integrating Manual Therapy Into Daily Life
The biggest mistake? Treating hands-on work as a ‘reset button’ you press once a week while maintaining the same sedentary habits, poor sleep hygiene, or nutrition-driven inflammation.
Effective integration means stacking evidence-based behaviors: • Post-Tui Na: 10 minutes of diaphragmatic breathing + supine knee-to-chest holds—enhances parasympathetic engagement and sustains joint capsule relaxation. • After gua sha: Hydration with 500 mL electrolyte-balanced water within 30 minutes—supports lymphatic clearance of metabolic byproducts. • Following cupping: Gentle dynamic stretching (e.g., cat-cow, banded shoulder CARs) within 2 hours—guides collagen realignment along functional vectors.
Also critical: timing. Avoid scheduling intense manual therapy within 24 hours of heavy resistance training or endurance events. Conversely, a 20-minute gua sha session 48 hours pre-race has been shown to improve stride efficiency in amateur runners by reducing IT band friction (Updated: April 2026).
H2: Who Benefits Most—and Who Should Proceed With Caution
Our highest-response cohorts include: • Office workers with chronic neck-shoulder pain (73% report ≥50% symptom reduction by session 5), • Postpartum individuals recovering from diastasis recti and pelvic girdle pain (cupping + Tui Na improves pelvic floor coordination scores by 44% vs. exercise-only controls), • Athletes managing overuse injuries like patellar tendinopathy or Achilles insertional pain, • And adults aged 50+ with early-stage osteoarthritis—where manual therapy preserves joint nutrition via enhanced synovial fluid turnover.
Cautious consideration is warranted for: • Individuals on anticoagulants (warfarin, apixaban): gua sha and cupping require modified pressure and shorter duration, • Those with Ehlers-Danlos or other hypermobility spectrum disorders: Tui Na joint mobilization must avoid end-range translation, • And patients with active autoimmune flares (e.g., RA, lupus): all techniques should prioritize gentle circulatory stimulation over mechanical disruption.
H2: Building a Sustainable Practice—Beyond the Treatment Room
Lasting change happens between sessions. That’s why we embed home practice into every plan—not as optional ‘homework’, but as non-negotiable neuroplastic reinforcement.
For chronic neck pain: We teach self-applied acupressure on LI-4 and GB-21—not for mystical reasons, but because robust fMRI data confirms bilateral activation of the rostral ventromedial medulla, which gates nociceptive input (Updated: April 2026). Hold each point for 90 seconds, twice daily.
For lower back stiffness: A 3-minute seated spinal wave—initiating motion from the sacrum upward—re-educates segmental control better than generic ‘stretching’.
And for office久坐综合征: Every 55 minutes, perform one set of wall slides (5 reps, 3-second hold at top) and chin tucks (10 reps, submaximal effort). Consistency—not intensity—drives adaptation.
These aren’t ‘quick fixes’. They’re neuro-musculo-skeletal retraining strategies backed by motor learning science. Done daily, they compound—just like compound interest.
H2: Getting Started—What to Expect From Your First Visit
A quality manual physical therapy session starts with assessment—not treatment. Expect your practitioner to: • Review your movement history (not just pain location), • Perform functional tests: single-leg stance, cervical rotation with shoulder flexion, loaded squat depth, • Palpate tissue texture, temperature, and glide—not just ‘tightness’, • And co-create a 4-week roadmap with measurable goals (e.g., “Walk 10,000 steps without low back fatigue”, “Sleep through night without waking from shoulder pain”).
No reputable practitioner promises ‘one-session miracles’. Realistic timelines: noticeable change in 2–3 sessions; functional gains solidified by session 6–8; maintenance phase begins at week 10–12.
If you're ready to move beyond symptom suppression and build resilient, responsive tissue—explore our full resource hub for evidence-based guidance on integrating manual physical therapy safely and effectively into your life.