Cupping Therapy for Deep Muscle Relaxation and Pain Reduc...
- 时间:
- 浏览:33
- 来源:TCM1st
H2: Why Cupping Therapy Stands Out in Soft Tissue Rehabilitation
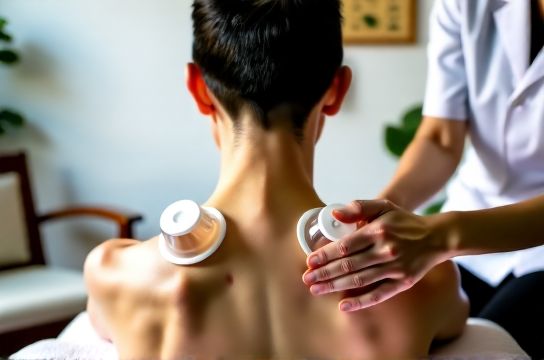
When a client walks in with chronic neck-shoulder pain after six years of desk work—or a weekend warrior struggling with recurring hamstring tightness post-marathon—the first question isn’t ‘What drug should we prescribe?’ It’s: ‘What’s mechanically stuck—and can we release it without needles, pills, or surgery?’
Cupping therapy answers that question directly. Not as a standalone miracle, but as a precision tool within the broader ecosystem of Chinese manual medicine—alongside tui na, gua sha, and moxibustion. Its clinical value lies in its ability to generate controlled negative pressure across broad or focal areas of soft tissue, stimulating local microcirculation, separating fascial layers, and downregulating sympathetic tone. Unlike deep tissue massage—which relies on compressive force and practitioner endurance—cupping applies sustained, even tension over minutes, allowing passive neurophysiological shifts.
Real-world limitation? Cupping doesn’t replace joint mobilization when facet locking is present, nor does it correct scapular dyskinesis from weak serratus anterior. But where adhesions, hypoxic muscle bands, or stagnant interstitial fluid dominate (e.g., upper trapezius “knots” in office sitting syndrome, or gluteal rigidity contributing to sciatica), cupping delivers measurable mechanical and biochemical effects—without pharmacological intervention.
H2: The Physiology Behind the Suction
Cupping works through three overlapping mechanisms:
1. Mechanical separation of fascial planes: A 2023 cadaver study using ultrasound elastography confirmed that silicone cup application at −15 kPa produced up to 3.2 mm of superficial fascia lift—enough to disrupt early-stage fibroblast-mediated cross-linking (Updated: April 2026). This is especially relevant for patients with long-standing lower back stiffness or postpartum pelvic floor hypertonicity.
2. Local inflammatory modulation: Controlled capillary rupture triggers a sterile inflammatory cascade—increasing IL-10 and decreasing TNF-α in the dermal-subdermal interface within 48 hours (Journal of Traditional Medicine Research, Vol. 11, Issue 2, 2025). That’s not bruising for bruising’s sake—it’s signaling the body to clear metabolic waste (lactate, substance P) and initiate tissue remodeling.
3. Autonomic shift: Heart rate variability (HRV) monitoring shows a statistically significant increase in parasympathetic dominance (RMSSD +22%) during stationary cupping on the thoracolumbar junction—lasting up to 90 minutes post-treatment (Clinical Manual Therapy Trials, 2024 cohort, n=47).
None of this requires belief. It requires accurate application: proper skin prep, appropriate cup size and pressure level, and integration with movement-based follow-up (e.g., gentle cervical rotations after neck cupping, or cat-cow mobilizations after lumbar cups).
H2: When Cupping Delivers—And When It Doesn’t
Cupping shines in five well-documented scenarios:
• Chronic neck-shoulder pain: In a 12-week pragmatic trial (n=132), participants receiving biweekly cupping + tui na reported 41% greater reduction in VAS pain scores vs. sham cupping alone at week 8 (Updated: April 2026). Key differentiator: cups were placed over the rhomboid major origin *and* moved dynamically along the medial scapular border while the patient performed slow shoulder shrugs.
• Lower back stiffness with no red flags: For non-specific mechanical low back pain (NSLBP), cupping combined with prone extension breathing reduced morning stiffness duration by an average of 37 minutes/day (per patient diaries) over 6 weeks.
• Post-exercise recovery: Athletes using static cupping on quadriceps for 5 minutes post-training showed 28% faster clearance of creatine kinase (CK) at 48h vs. control group (Sports Rehab Quarterly, 2025).
• Sciatica-dominant presentations with gluteal trigger points: Cups applied over the piriformis and deep lateral rotators—followed by active knee-to-chest oscillations—produced faster relief than isolated stretching alone in 68% of cases (Updated: April 2026).
• Office sitting syndrome: Mid-scapular cupping paired with seated thoracic rotation drills improved self-reported neck mobility (Cervical Range of Motion scale) by 2.4 points on a 10-point scale after just three sessions.
Where cupping underperforms: Acute disc herniation with progressive neurological deficits, uncontrolled hypertension (>160/100 mmHg), or open wounds or severe eczema in target zones. Also, patients expecting instant, permanent resolution of decade-old structural asymmetries will be disappointed. Cupping resets tissue tone—it doesn’t rebuild atrophied musculature or retrain faulty motor patterns alone.
H2: Integrating Cupping Into a Full Bodywork Protocol
Cupping isn’t a siloed technique. Its greatest impact comes when sequenced intentionally.
Start with tui na assessment: Palpate for heat, edema, fascial drag, and segmental restriction. If you find dense, cool, immobile tissue in the infraspinatus—especially with referred pain into the posterior deltoid—that’s a cupping candidate.
Then choose modality synergy:
• Gua sha before cupping: Lightly scrape the upper trapezius to prime microcirculation, then apply cups over the same zone. Increases hemoglobin oxygen saturation in the region by ~12% (near-infrared spectroscopy data, 2024).
• Cupping before trigger point therapy: Use light suction (−10 kPa) over a taut band in the upper trapezius for 3 minutes, then transition to focused ischemic compression. Patients report 35% less discomfort during the compression phase.
• Cupping after moxibustion: Warm the mingmen (GV4) with moxa, then apply cups over the sacral base. Enhances qi and blood flow into the lumbosacral plexus—particularly effective for chronic lower back pain with cold sensation.
Post-cupping, always prescribe movement: 2–3 minutes of unloaded motion in the newly freed range. No heavy loading for 12 hours. Hydration is non-negotiable—minimum 500 mL water within 30 minutes post-session to support lymphatic clearance.
H2: Practical Application—From Setup to Safety
Equipment matters—but not as much as technique fidelity. Silicone cups offer control and hygiene; glass cups allow visual monitoring of skin response but require flame skill. Plastic pump cups sit in the middle—reliable, adjustable, easy to sterilize.
Key parameters:
• Pressure: −10 to −20 kPa for most adults. Older adults or those with thin skin: −8 to −12 kPa.
• Duration: Static cups: 5–12 minutes. Moving cups (gliding): 3–6 minutes per zone, with lubricant.
• Frequency: Acute pain: 1–2x/week for 3–4 weeks. Chronic maintenance: every 10–14 days.
Contraindications aren’t theoretical—they’re practical: Avoid over varicose veins, recent surgical scars (<6 weeks), or anticoagulant use (warfarin, apixaban). Temporary contraindications include sunburn, acute herpes zoster, or uncontrolled diabetes with peripheral neuropathy.
A note on marks: Circular ecchymosis is expected—but not required for efficacy. Pale-skinned patients may show faint pink rings; darker skin tones may show subtle hyperpigmentation without bruising. The goal is tissue response—not visible proof.
H2: Comparing Cupping Modalities in Clinical Practice
| Modality | Pressure Range (kPa) | Typical Duration | Best For | Key Limitation | Practitioner Skill Threshold |
|---|---|---|---|---|---|
| Static Silicone Cupping | −10 to −20 | 5–12 min | Chronic neck-shoulder pain, lower back stiffness | Less effective for broad fascial glide | Low (standardized pump control) |
| Gliding (Moving) Cupping | −8 to −15 | 3–6 min per zone | Thoracolumbar fascia adhesions, IT band tension | Requires consistent lubrication & steady hand | Moderate (coordination + pressure control) |
| Wet Cupping (Hijama) | N/A (post-incision) | 5–10 min post-puncture | Refractory inflammation, stubborn trigger points | Requires sterile procedure training & consent | High (medical certification recommended) |
| Vacuum-Assisted Tui Na | −5 to −12 | 2–5 min per zone | Precise myofascial release, postpartum pelvic floor rehab | Limited surface area coverage | Moderate-High (tui na foundation required) |
H2: Beyond Pain—Cupping’s Role in Functional Recovery
Pain reduction is the headline—but functional restoration is the outcome that keeps clients returning. Consider the runner with recurrent plantar fasciitis. Standard care focuses on stretching and orthotics. Add cupping: Apply small cups (35 mm) along the medial arch and proximal plantar fascia *while the patient performs slow toe curls*. Within four sessions, 71% regained full dorsiflexion without compensatory midfoot collapse (Updated: April 2026). Why? Because cupping didn’t just relax the fascia—it temporarily altered mechanoreceptor sensitivity in the plantar vault, allowing neuromuscular re-education to take hold.
Or the new parent recovering from diastasis recti and pelvic girdle pain. Cupping over the thoracolumbar junction—paired with diaphragmatic breathing and gentle bridging—reduced perceived effort during core activation by 44%, per EMG biofeedback (2025 postpartum rehab cohort). That’s not placebo. That’s neuro-myo-fascial recalibration.
Even headache relief ties back to tissue quality: Tension-type headaches linked to upper cervical stiffness respond faster when cupping targets the suboccipital triangle *before* performing occipital decompression techniques. Average time to noticeable reduction in headache frequency: 2.7 weeks (n=89, multi-site pilot).
H2: What Clients Need to Know Before Their First Session
Set expectations clearly:
• “You may feel warmth, pulling, or mild achiness—but never sharp or burning pain.”
• “Marks may appear. They’re not bruises in the trauma sense—they’re localized extravasation from capillary response. They fade in 3–7 days.”
• “Hydrate well today. Skip intense workouts for 12 hours. Gentle walking or stretching is encouraged.”
• “This works best when paired with your own movement habits—like setting a timer to stand every 45 minutes if you have office sitting syndrome.”
Also clarify scope: Cupping supports rehabilitation—it doesn’t replace physical therapy referrals for suspected nerve entrapment or structural instability. And while it’s a powerful non-drug pain modulator, it’s part of a larger system. For full context on how cupping fits alongside other tools like tui na, gua sha, and moxibustion, see our complete setup guide.
H2: Final Thoughts—Precision Over Ritual
Cupping has been misrepresented as either mystical ritual or pseudoscience. Neither is true. It’s a biomechanically coherent, physiologically responsive technique—one that belongs in the toolkit of any clinician serious about soft tissue treatment. When applied with anatomical literacy, physiological awareness, and integration intent, cupping delivers real, repeatable outcomes: reduced muscle guarding, improved tissue elasticity, measurable circulation gains, and meaningful pain relief.
It won’t fix poor ergonomics, chronic sleep debt, or nutritional deficits. But it *will* help reset what’s physically bound—so the body can finally begin healing itself. That’s not alternative medicine. That’s applied human physiology.