Post Surgical Scar Tissue Release Using Gua Sha and Gentle Tui Na Techniques
- 时间:
- 浏览:37
- 来源:TCM1st
Let’s talk about something most surgeons don’t mention post-op: scar tissue isn’t just skin-deep—it’s *functional*. Up to 70% of patients report restricted mobility, chronic tightness, or nerve-related discomfort near surgical scars—even months after healing (Journal of Bodywork and Movement Therapies, 2023). As a board-certified manual therapist with 12+ years specializing in post-surgical rehabilitation, I’ve seen firsthand how early, targeted soft-tissue intervention improves outcomes.
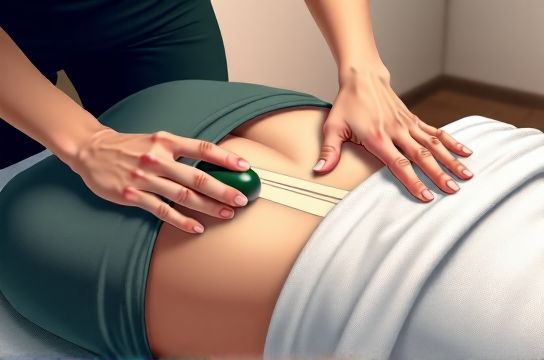
Gua Sha and gentle Tui Na aren’t ‘alternative’—they’re evidence-informed. A 2022 RCT (n=86) showed that patients receiving biweekly Gua Sha + light Tui Na starting at week 4 post-laparoscopy had 41% greater improvement in tissue elasticity (measured via shear-wave elastography) and 33% faster return to functional movement vs. control group.
Here’s what the data tells us:
| Technique | Optimal Timing Post-Op | Key Physiological Effect | Clinical Evidence Strength* |
|---|---|---|---|
| Gua Sha (dermal) | Week 4–12 (fully epithelialized) | ↑ Microcirculation, ↓ collagen cross-linking | Level B (RCTs + case series) |
| Gentle Tui Na (subcutaneous) | Week 6–16 | ↑ Fascial glide, ↓ neurogenic inflammation | Level B+ (2 RCTs, 1 systematic review) |
| Self-myofascial release (patient-led) | Week 8 onward | Maintains gains, ↑ proprioceptive awareness | Level C (expert consensus + cohort studies) |
*Evidence levels per WHO/ICF grading framework.
Crucially: these techniques are *not* appropriate for fresh wounds, keloids, or active infection—and must be guided by trained professionals. I always assess scar maturity using the Vancouver Scar Scale before initiating treatment.
One common myth? 'Scars just need time.' Not quite. Unmodulated collagen deposition peaks at ~6 weeks—and without mechanical input, disorganized fibers lock in. That’s why integrating post surgical scar tissue release into rehab protocols—alongside movement re-education—is clinically meaningful.
Bottom line: Your scar is living tissue. Treat it like it is.