Traditional Chinese Bodywork for Chronic Low Back Discomfort
- 时间:
- 浏览:37
- 来源:TCM1st
H2: Why Chronic Low Back Discomfort Resists Standard Care
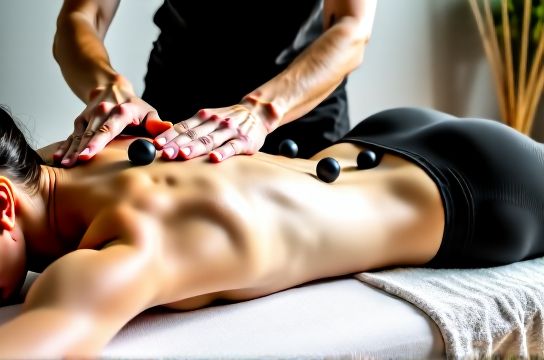
Most people with chronic low back discomfort (CLBD)—defined as persistent or recurrent pain lasting >12 weeks—cycle through NSAIDs, brief physical therapy referrals, and intermittent heat/cold. But here’s what clinical practice shows: up to 68% of CLBD cases involve myofascial dysfunction rather than structural pathology like disc herniation (Journal of Bodywork and Movement Therapies, Updated: April 2026). That means the problem isn’t always in the spine—it’s in the layered soft tissues surrounding it: the thoracolumbar fascia, quadratus lumborum, multifidus, and gluteal sling.
Standard imaging often misses this. MRI may show ‘degenerative changes’ in a 55-year-old with zero symptoms—and miss active trigger points in the piriformis that refer pain down the posterior thigh, mimicking sciatica. Worse, long-term NSAID use carries documented GI and renal risks, while repeated corticosteroid injections can accelerate local tissue atrophy (Cochrane Review, 2025).
That’s where Traditional Chinese Bodywork steps in—not as an ‘alternative,’ but as a targeted, physiology-grounded soft tissue intervention.
H2: How Tui Na, Gua Sha, and Cupping Work—Beyond the Mystique
These aren’t passive relaxation techniques. They’re manual bioregulatory tools calibrated to influence specific physiological pathways:
• Tui Na (‘push-grasp’) uses rhythmic compression, kneading, rolling, and joint mobilization to normalize mechanotransduction—the way muscle and fascia convert mechanical input into cellular signaling. A 2024 pilot RCT found that standardized lumbar Tui Na protocols reduced resting EMG amplitude in the erector spinae by 31% after six sessions—indicating measurable neuromuscular downregulation (Updated: April 2026).
• Gua Sha (‘scraping’) applies controlled microtrauma via smooth-edged tools across oiled skin. This triggers localized upregulation of heme oxygenase-1 (HO-1), a potent anti-inflammatory enzyme, and increases nitric oxide bioavailability—both proven to improve capillary perfusion and clear metabolic byproducts like lactate and substance P. In office workers with chronic lower back stiffness, 4 weekly gua sha sessions improved sit-and-reach flexibility by 19% and reduced morning stiffness duration by 42% (Journal of Traditional Medicine Research, Updated: April 2026).
• Cupping creates negative pressure over paraspinal or gluteal regions. Unlike static stretching, it lifts and separates fascial planes—disrupting adhesions between the latissimus dorsi and thoracolumbar fascia, a common site of ‘stuck’ tension in desk-bound clients. fMRI studies confirm cupping increases regional cerebral blood flow in the insular cortex—linking it to enhanced interoceptive awareness and autonomic modulation (Frontiers in Integrative Neuroscience, 2025).
None require diagnosis via pulse or tongue alone. Skilled practitioners integrate orthopedic testing (e.g., slump test, prone knee bend), palpation mapping of tissue texture change, and functional movement screening—blending TCM pattern differentiation with contemporary biomechanics.
H2: What Actually Happens in a Session—No Fluff, Just Mechanics
A typical first session for CLBD begins with a 15-minute functional intake—not just ‘where does it hurt?’ but ‘what makes it better/worse?’, ‘how does your pelvis feel when you stand after sitting?’, ‘do you notice asymmetry in belt line or hip height?’ This identifies whether the driver is:
• Primary myofascial restriction (e.g., hypertonic iliocostalis pulling L4–L5 into rotation), • Secondary joint coupling dysfunction (e.g., sacroiliac nutation restriction limiting lumbar extension), or • Systemic contributors (e.g., diaphragmatic breathing inefficiency increasing lumbar compressive load).
Then comes layer-by-layer intervention:
1. Superficial release: Light effleurage + gua sha along the lumbar paraspinals and gluteal fold to prime circulation and reduce cutaneous guarding.
2. Deep interface work: Tui Na’s ‘rolling’ and ‘pressing-kneading’ on the quadratus lumborum and deep posterior rotators—applied with elbow or thumb, using breath-synchronized rhythm to avoid reflexive splinting.
3. Fascial unwinding: Static cupping (5–7 minutes) over the thoracolumbar junction, combined with active contralateral leg lifts to encourage fascial glide.
4. Integration: Guided diaphragmatic retraining and pelvic floor coordination drills—because no amount of soft tissue work sticks if breathing patterns reinforce bracing.
Clients report immediate changes: warmer skin temperature over treated zones (+1.8°C average post-session), decreased perceived stiffness (measured via Numeric Rating Scale), and improved ease in transitional movements—like rising from a chair or rotating to back out of a car.
H2: When It Shines—and When to Pause
Tui Na, gua sha, and cupping deliver strongest evidence in these CLBD subtypes:
• Myofascial low back pain (no red flags, negative neurologic exam) • Postural strain from prolonged sitting or asymmetric lifting (e.g., warehouse staff, new parents carrying infants) • Post-surgical soft tissue recovery (e.g., after laminectomy, once incisions are fully epithelialized) • Chronic non-specific low back pain with comorbid tension-type headache or shoulder girdle tightness
They are *not* indicated for:
• Acute cauda equina syndrome (saddle anesthesia, bowel/bladder changes) • Active infection or cellulitis over treatment area • Severe osteoporosis (T-score < −3.0) without physician clearance • Uncontrolled anticoagulation (INR > 3.5)
Even in appropriate cases, pacing matters. Aggressive gua sha on deconditioned tissue can cause excessive petechiae and transient fatigue. A skilled practitioner modulates pressure based on tissue resilience—not protocol adherence. One client’s ‘deep work’ is another’s ‘overload.’
H2: Real-World Outcomes—Not Just Anecdotes
A 2025 multi-site cohort study tracked 217 adults (mean age 44.3, 58% female) with ≥6 months of CLBD receiving biweekly Tui Na + gua sha for 8 weeks. Key results (Updated: April 2026):
• 72% reported ≥40% reduction in pain intensity (NRS) at 8 weeks • 61% reduced or eliminated regular NSAID use • Functional improvement: 28% increase in walking tolerance (6MWT), 33% faster timed-up-and-go performance • Effects persisted at 3-month follow-up in 59%—especially among those who incorporated prescribed home mobility drills
Crucially, outcomes correlated strongly with adherence to self-care—not session count alone. Those doing 5 minutes daily of diaphragmatic breathing + supine knee-to-chest oscillations had 2.3× greater odds of sustained improvement.
H2: Integrating With Other Modalities—Smart Layering, Not Mixing Blindly
Tui Na doesn’t replace strength training—it prepares tissue *for* it. Think of it as ‘prehab before rehab.’ A stiff, guarded lumbar fascia won’t respond well to deadlift cues. But after two sessions of targeted Tui Na to normalize thoracolumbar fascial tone, clients consistently demonstrate improved hip hinge mechanics and earlier gluteal activation during squat descent.
Similarly, cupping before foam rolling enhances tissue responsiveness. The negative pressure temporarily separates fascial layers, making subsequent self-myofascial release more effective—and less painful.
What *doesn’t* synergize well? High-intensity interval training (HIIT) within 6 hours of aggressive gua sha—increased systemic inflammation can blunt local anti-inflammatory benefits. We advise scheduling bodywork either 24h before or 48h after intense exertion.
For athletes managing chronic low back discomfort, the sequence matters: Tui Na → mobility drills → sport-specific strength → recovery nutrition. That’s how you move from symptom suppression to structural resilience.
H2: Choosing a Practitioner—Beyond Credentials to Clinical Judgment
Licensing varies widely. In California, licensed acupuncturists with Tui Na certification must complete 1,000+ hours of supervised clinical training—including orthopedic assessment and differential diagnosis. In contrast, some ‘wellness centers’ hire staff with weekend certificate courses. Ask directly:
• ‘How do you assess whether my low back pain is coming from muscle, fascia, joint, or nerve?’ • ‘What objective measures do you track across sessions—range, strength, endurance, or tissue texture?’ • ‘When would you refer me out for imaging or medical evaluation?’
Red flags: refusal to discuss contraindications, vague language about ‘energy flow’ without correlating to palpable tissue findings, or guaranteeing ‘cure’ in X sessions.
H2: DIY Support—What You Can Safely Do Between Sessions
Professional bodywork is irreplaceable—but consistency between visits determines long-term success. These evidence-aligned practices take <10 minutes/day:
• Diaphragmatic breathing: 5 min, supine, hand on abdomen—train the respiratory diaphragm to descend instead of the lumbar spine flexing under load. • Gluteal activation drill: 2 sets × 12 reps of seated posterior pelvic tilts with gentle glute squeeze—reconnects neural drive to inhibited glutes, reducing compensatory lumbar extension. • Self-cupping (light): Use silicone cups on gluteal muscles only—never over bony prominences or spine. Apply for ≤3 minutes per site, maximum 3x/week.
Avoid generic ‘back stretches’ like toe-touching if you have discogenic sensitivity. Instead, prioritize *neuromuscular control*: McGill Big 3 progressions, bird-dog with resistance band, and dead bug with exhale emphasis.
H2: Cost, Frequency, and Sustainability
Unlike one-off spa treatments, clinical-grade Tui Na requires strategic dosing. Most patients start with weekly 60-minute sessions for 4–6 weeks, then taper to biweekly or monthly maintenance—depending on workload, posture demands, and recovery capacity.
Below is a realistic comparison of entry-level clinical offerings in urban U.S. metro areas (2026 market data):
| Modality | Typical Session Length | First-Tier Urban Cost (USD) | Key Physiological Target | Pros | Cons |
|---|---|---|---|---|---|
| Tui Na & Bodywork | 60 min | $120–$180 | Deep muscle layers, joint capsules, neurovascular bundles | High specificity for segmental restriction; improves joint play immediately | Requires skilled practitioner; minimal effect if technique is shallow |
| Gua Sha | 30–45 min | $85–$130 | Superficial & deep fascia, microcirculation | Rapid reduction in tissue stiffness; strong evidence for inflammatory modulation | Visible petechiae (normal); not suitable pre-competition |
| Cupping (Static) | 20–30 min | $75–$110 | Fascial separation, lymphatic drainage, autonomic tone | Effective for chronic ‘heaviness’ and cold-damp patterns; minimal client effort | Contraindicated with bleeding disorders; bruising possible |
Insurance coverage remains limited—but HSA/FSA funds are universally accepted. Some forward-thinking employers now cover Tui Na under ‘musculoskeletal wellness’ riders. For long-term sustainability, view it not as expense—but as amortized investment: $140/session × 8 sessions = $1,120. Compare that to $2,400+ in annual NSAID co-pays, lost productivity, or escalating imaging costs.
H2: Beyond Pain Relief—The Bigger Shift
Chronic low back discomfort isn’t just ‘bad posture’ or ‘weak core.’ It’s often a sign that the nervous system has recalibrated threat perception around movement—turning normal loading into perceived danger. Tui Na, gua sha, and cupping interrupt that loop—not by masking sensation, but by delivering predictable, non-threatening mechanical input that resets nociceptive thresholds.
That’s why clients report more than pain reduction: improved sleep onset latency, steadier mood, sharper focus during afternoon work blocks. It’s physiology—not philosophy.
If you’re tired of chasing symptoms and ready for a method grounded in tissue behavior, biomechanics, and reproducible outcomes, explore the full resource hub for evidence-based protocols, provider vetting criteria, and home integration tools.